
My 85-year-old father loved people, and he waved hello to everyone as he tooled around his Escondido assisted-living facility in his tricked-out electric wheelchair. He couldn’t resist talking to a neighbor at his doorway when the building went off pandemic lockdown a few weeks ago. They couldn’t hear each other, so they pulled off their masks for a quick chat. How-are-ya, fine-thanks. What a year!
Maybe that was the moment the germs slipped into his chest.
Perhaps one of the caregivers brought the coronavirus into his apartment from the outside. Or he could have been infected when he visited the hospital for a vascular test.
We’ll never know for sure. It is clear, however, that COVID-19 found its way to my father and took his life. But not before a long, complicated and agonizing cascade of medical complications that left him exhausted, alone and afraid.
Novelist Philip Roth wrote that “old age is a massacre.” It’s got nothing on the horrible effects of a new deadly combo – isolation, hospitalization and the coronavirus. Unfortunately, thanks to our national and local failures, more San Diegans are destined to die like my dad.
The Rock of Our Family Gets a Positive Test
The story of how my parents met is literally a tall tale.
In the late 1960s, Ralph Dotinga – the son of Dutch immigrant dairy farmers – was a 6-foot-6 teacher at a Chula Vista elementary school. The ladies in the faculty lounge noticed his height and coaxed him to sit next to a fetching 5-foot-10 colleague with an unusual name. They knew what they were doing: It didn’t take long for Ralph and Sudelle to both invite their classes to their wedding.
Dad would go on to have two sons with Mom and teach elementary school for more than 30 years. After the local news reported on his death, two students from his fifth-grade class in 1960 separately reached out to me about his legacy: “There must be many hundreds of people out there who will always recall him with admiration and thanks,” one wrote.
At home, Dad was the rock of our zany and complicated family, the anchor who kept us from running aground as we navigated rough waters. The health problems and the endless hospital visits came late in life after a pleasant retirement in Oceanside overlooking a golf course he loved to visit.
Somehow, he survived two heart attacks, one cardiac arrest, a quadruple bypass, diabetes and crippling falls. Pretty soon, I predicted, they’d name a hospital wing after us. Funny, he said.
Nonetheless, to borrow a phrase, he persisted.
About a week before Thanksgiving, Dad fell and went by ambulance to Palomar Medical Center in Escondido. He’d cracked a bone in his knee and couldn’t stand up. The hospital got ready to send him to a skilled nursing home for rehab to get back on his feet – a drill he’d been through multiple times before. But first they gave him a coronavirus test. It was positive.
This was the beginning of the end.
Isolated and Alone, the Complication Cascade Begins
Dad had no symptoms then, but he was stuck in the hospital. Only a pair of skilled nursing homes in the county would accept COVID-positive patients. They were full, we learned, or didn’t return phone calls.
San Diego County is home to 3.2 million people, roughly the population of Utah or Connecticut, and not a single nursing-home bed was available for my father. Then again, maybe we dodged a bullet. Those two COVID-friendly nursing homes had gotten bad press: “El Cajon Nursing Home Reaped Big Profits While Shortchanging Resident Care, Analysis Shows,” read the October headline about one of them. The other nursing home needed assistance from the National Guard when COVID-19 overwhelmed its staff in November.
A few days passed, then Dad complained that the hospital food was more terrible than usual. His sense of taste was out of whack, a classic sign of COVID. COVID pneumonia soon set in as his oxygenation level dipped. He didn’t need a ventilator, but he went on oxygen and began a remdesivir-steroid regimen. No expensive fancy drugs for my father, though. He’s not the president.
Dad remained in good spirits for the most part, and he started reminiscing about his life. “I love your mother as much as anyone could love someone,” he said. “He must be delirious,” Mom joked when I told her. My response: “That’s what I said!”
Mom, unfortunately, was in for her own struggles amid a massive coronavirus outbreak at the assisted-living facility. About a week after Dad went to the hospital, a brutal bout with COVID-19 left Mom afraid for her life and almost too weak to stand. A widow now, she’s still recovering.
Back at the hospital, Dad came down with a blood infection with MRSA, the horrific superbug that hangs around medical facilities. As patients and families learn every day, it’s dangerous to be extremely sick in a place full of germs.
The medical team installed a long-term intravenous line to administer an antibiotic for six weeks. Then disorientation set in.
A Text with a Single Word: ‘Help’
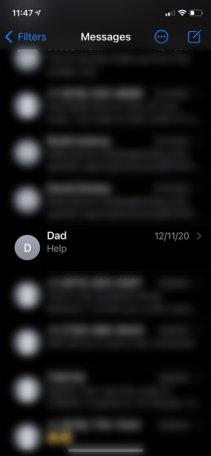
Dad called me three times at 4 a.m. one day to ask me to call 911 for him; another time he texted a single word — “help” — to me from Room 993. I’d never seen him send a text before.
He was fine, his nurses said, just confused. I don’t know if they comforted him or held his hand. In the era of coronavirus, we couldn’t be there at all.
Delirium and disorientation are common in people who are hospitalized, and they’re especially common in isolated patients with COVID-19 who are treated by medical professionals with their faces covered by masks, shields and goggles. “This is a perfect storm for delirium. The best thing is to get them out of the hospital and into familiar surroundings,” said hospital physician Dr. Charlie Wray of the University of California at San Francisco, in an interview. “But when people stay in the hospital for prolonged periods of time, we often tend to find more reasons to keep them there.”
He means that complications crop up like Dad’s MRSA blood infection.
The pneumonia cleared up after a few days but my dad remained positive for coronavirus so he couldn’t leave for a nursing home to get rehab for his leg. The two COVID-friendly facilities still weren’t available. Meanwhile, his muscles deteriorated since he was still unable to get out of bed on his own.
Weeks passed, and more complications appeared. The hospital put him on blood thinners to prevent COVID-related blood clots, but he had bleeding and bruising, and they stopped the regimen. Then he had a urinary blockage that caused pain until they removed two liters of urine via a catheter. He became so drowsy that nurses new to him never got to see the warmth and charm – “what a sweet man!” – that their colleagues spoke about weeks earlier.
After Almost Five Weeks, the End of a Story
Dad spent much of his last week asleep. Three nights before Christmas, he wouldn’t wake up when they tried to rouse him. Tests didn’t reveal a cause. The hospitalist – a physician who oversees cases at hospitals – talked to me about what we would want for him if things didn’t improve. He hoped my dad might respond to a medication for his suddenly abnormal liver levels, one that would be given through a nasogastric tube. I approved giving it to him since it wasn’t deeply invasive. But Dad passed away around 2 a.m. as the team prepared to administer the drug.
The physician gave me the news over the phone. I then called my mother and brother to tell them that Dad had just passed away.
My father’s death certificate says COVID-19 is the cause of death. It appears to have caused a fatal stroke – one of the things the virus does.
Dad was at the hospital for just shy of five weeks, alone the entire time. This is no way to live, and no way to die.
The Cost of Endless Hospitalization
This kind of endless saga isn’t unusual. Not everyone in the hospital with COVID-19 lives to tell the tale or dies after going on a ventilator. Some stay longer than a month, making it more likely that they’ll get other diseases like hospital infections and suffer from the effects of not moving around like loss of muscle tone. And the lack of space in nursing homes means that hospitals can’t discharge patients when they’re ready to leave.
“If someone occupies a room for two to three weeks recovering from a disease, that’s two to three weeks in which that hospital doesn’t have that bed,” Wray said. “That’s longer than what usually happens, and that’s a complicating factor in this pandemic that a lot of people don’t fully understand. Simply put, we’ve got the spigot on, filling up the tub, while the drain is partially plugged.”
Dad is now waiting to be cremated and laid to rest. He is one of more than 1,800 people who have died in San Diego County of COVID-19. The pandemic has taken more than 29,500 lives in California — more than the population of Coronado or Lemon Grove.
“You Are More Likely to Die From a Lightning Strike’
Some people will say my father was old and sick and due for death. County Supervisor Jim Desmond, for instance, has claimed that most COVID-19 deaths aren’t “pure.” Yes, supervisor, Dad had a very important pre-existing condition: He was alive. And then, thanks to COVID-19, he wasn’t.
There’s also this fact: The coronavirus worked so hard to take my dad’s life that it seems like he had more time to live, to be a husband and father and friend. Ending this way – stuck in a hospital, isolated and robbed of human touch – is so brutal and so needless. And so undeserved for anyone, let alone a kind, sweet man known for his generosity of spirit.
We’ve been failed by so many careless people who’ve allowed this pandemic to grow and kill so many: The vapid politicians, starting at the top. The cruel and heartless local Skyline megachurch, which we attended when I was a kid, whose website lies that “you more likely to die from a lightning strike than the Covid-19 virus.” And the craven business owners, apathetic partiers and diners, and selfish anti-maskers. There’s no limit to their lack of caring for the vulnerable.
I’m my dad’s son, and I’m generally good-natured just like him. Anger always seems unnatural to me, and I usually can’t sustain it for long. But if enough people get furious and stay furious, maybe we can make this stop.
It will be expensive, and it will be hard. So what? I’m hardly the first to say this, but I know it now more than ever: The cost we’re paying is more than we can bear.
A version of this article appeared earlier on the medical news site MedPage Today.

